Posts Tagged ‘UNC’
A nuclear power scare from Japan
Sunday, March 27, 2011, 11:12 pm No Comments | Post a CommentThe hydrogen explosions, the fire, the radioactive leaks and the evacuations at the earthquake- and tsunami-ravaged Fukushima Daiichi nuclear plant about 150 miles north of Tokyo happened a continent and an ocean away from North Carolina’s Research Triangle. But there’s a good chance the fallout from the nuclear crisis in Japan will hit close to home - lest you forget the Shearon Harris nuclear plant about 20 miles southwest of Raleigh.
On clear days, Shearon Harris’ cooling tower and the steam rising from it are clearly visible across the Triangle, even from Eno River State Park about 50 miles north. Splitting an atom, a process called nuclear fission, is cleaner than burning coal to generate electricity and Progress Energy, which operates Shearon Harris, plans to add two reactors to the existing one by 2018.
But the events at the Fukushima Daiichi nuclear power plant could delay expansion plans at Shearon Harris and elsewhere in the U.S. and make them more expensive.
The Japanese earthquake and its fallout “will slow nuclear power down in the U.S.,” Paul Turinsky, professor of nuclear engineering, said during a symposium Wednesday at N.C. State University. Turinsky was one of four NCSU experts who spoke at the symposium.
The same day, the Nuclear Regulatory Commission and the nuclear power industry agreed to reassess reactor designs and training procedures and to reevaluate reactors at the 104 operating nuclear power plants nationwide.

The Chernobyl reactor was an open design, lacking steel and concrete to contain radioactive material in case of an accident.
Also, public support for more nuclear energy has dropped. According to a CBS poll, more Americans disapproved than approved of building more nuclear plants in the wake of the Fukushima Daiichi crisis, and for the first time since the 1986 nuclear disaster in Chernobyl the disapproval rate reached 50 percent.
Add to that regulatory shortcomings fueling anti-nuclear sentiment that has lingered since the Three Mile Island nuclear power plant accident in 1979 and has foiled three decades worth of attempts to establish a nuclear waste repository.
A 2010 report by the Union of Concerned Scientists listed 27 cases in which nuclear power plants accidentally released radioactive materials over the previous four years and the Nuclear Regulatory Commission allowed plant owners to violate regulations with impunity.

A pressurized water reactor like the one at Shearon Harris has a steel vessel around the reactor core and concrete containment structures.
Seven of the 27 violations happened at nuclear plants in North Carolina. Shearon Harris accounted for two of the seven; radioactively contaminated water leaked into the ground in both cases.
With Triangle residents following updates on the nuclear crisis in Japan, Triangle universities scrambled to line up nuclear energy experts who tried to dispel fears with facts. The day following the NCSU symposium, the University of North Carolina’s Morehead Planetarium and Science Center hosted a talk by David McNellis, the director of UNC’s Center for Sustainable Energy, Environment and Economic Development, on the risks of nuclear power.
Back to back, the experts analyzed nuclear reactor designs and their failures, from Three Mile Island to Chernobyl to Fukushima Daiichi.
Based on estimates of how much the general public was exposed to radioactively contaminated material, Man-Sung Yim, an associate professor of nuclear engineering and a radiological health expert at NCSU, ranked Chernobyl as the worst of the three nuclear power plant failures.

The Fukushima Daiichi plant uses boiling water reactors, which are equipped with steel reactor vessels and concrete containment structures.
Radiation exposure from Fukushima Daiichi “is less than Chernobyl, but far worse than Three Mile Island,” Yim said during the NCSU symposium.
Based on published measurements, Yim calculated that the general population was exposed to about 33 rem of radiation in Chernobyl. The evacuated area around the Fukushima Daiichi plant has received a dose of up to 10 rem.
The Three Mile Island accident exposed the general public to about 180 millirem of radiation, less than the 300 millirem to 600 millirem of radiation Americans take in every year from everyday living.
A 400 rem dose of radiation is considered lethal, Yim said.
The other experts linked the exposure risk of the three nuclear power plant failures directly to reactor design and operational safety standards.
All nuclear power plants generate electricity from steam that turns a turbine linked to a generator. The heat needed to turn water into steam comes from nuclear fission.

John Gilligan, professor of nuclear engineering at NCSU, shows off a nuclear fuel rod at the symposium.
The fuel to produce the heat is uranium, a natural metallic element in rock, soil and water that comes in multiple versions. The uranium is contained in ceramic-like pellets that are stacked in fuel rods in the core of a reactor. One uranium version, uranium-235, breaks apart when it gets hit by a neutron, releasing two to three neutrons, two radioactive fission products and heat. When released neutrons hit more uranium-235, the nuclear fission continues as a chain reaction.
Unlike the Three Mile Island and Fukushima Daiichi nuclear power plants, the Chernobyl nuclear power plant had no steel vessels around its reactor cores. When an experiment went awry on April 26, 1986, and reactor No. 4 overheated, pressure from the steam continued to build until it blew off the roof of the reactor building, scattering radioactive material from the melting reactor core across the landscape and setting free radioactive clouds that drifted westwards.
The Fukushima Daiichi plant withstood the massive March 11 earthquake, even though it wasn’t designed for such a powerful seismic event, John Gilligan, professor of nuclear engineering, said during the NCSU symposium.
Control rods automatically stopped nuclear fission, in effect shutting down reactors that were in operation the moment the electricity supply to the plant was cut off.
“It wasn’t the earthquake,” that caused the nuclear crisis at Fukushima Daiichi, Michael Doster, professor of nuclear engineering at NCSU, said. “It was the tsunami.”
The wall of water the earthquake had unleashed was more than twice as tall as the floodwall that was supposed to protect the nuclear power plant facing the sea. When the water flooded the plant, it knocked out emergency diesel engines that powered pumps, fans and other electrical equipment in the reactor buildings. After about eight hours, batteries backing up the emergency diesel engines were also exhausted.
Without power, pumps stopped cooling the water in 40-foot-deep pools that held spent fuel rods. The rods usually stay in these pools for about five years during which time they continue to give off heat. But unlike in the reactor, the heat production in the spent fuel storage pools cannot be turned off, said Doster.
“You cannot avoid it. You cannot control it,” he said. “You just have to deal with it.”
The spent fuel rods in the Fukushima Daiichi storage pools are made from zirconium alloy. As the temperature continued to rise in the storage pools, the zirconium interacted with the heated water and produced hydrogen gas. It was that hydrogen gas that exploded, Doster said. The explosions damaged the concrete buildings of at least two of the reactors and released radioactive material from the spent fuel.
Design flaws, malfunctioning equipment and human error caused reactor No. 2 at the Three Mile Island nuclear power plant to overheat March 28, 1979, UNC’s McNellis said.
It was the worst commercial nuclear power plant accident in U.S. history and led to sweeping changes involving emergency response planning, reactor operator training, human factors engineering, radiation protection and many other areas of nuclear power plant operations, according to the NRC. Regulatory oversight also tightened to enhance safety.
 Like two-thirds of U.S. nuclear power plants, Shearon Harris’ reactor is the same design as reactor No. 2 at Three Mile Island. The remaining one-third of U.S. nuclear power plants rely on boiling water reactors like the Fukushima Daiichi plant.
Like two-thirds of U.S. nuclear power plants, Shearon Harris’ reactor is the same design as reactor No. 2 at Three Mile Island. The remaining one-third of U.S. nuclear power plants rely on boiling water reactors like the Fukushima Daiichi plant.
Shearon Harris became operational in 1987, eight years after the Three Mile Island triggered the regulatory and safety changes.
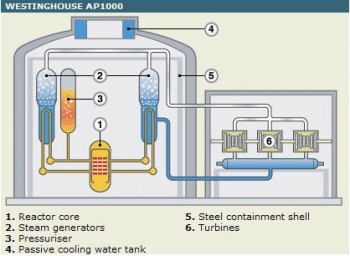
The two reactors Progress Energy has proposed to add at Shearon Harris are a new design. Called AP1000, it includes a cooling tank on top of the reactor from which water trickles onto the core without the need for pumps.
Construction of nuclear plants with AP1000 reactors have begun in China and the U.S.
Charlotte-based Duke Energy, which is buying Raleigh-based Progress Energy, plans to build a nuclear power plant with AP1000 reactors in South Carolina. More are proposed in Florida and Alabama.
(Watch a video of the NCSU symposium here.)
Expanding the Hamner one institute at a time
Monday, March 21, 2011, 11:03 pm No Comments | Post a CommentWilliam Greenlee is getting ready to build another institute on the 56-acre campus of the Hamner Institutes for Health Sciences in Research Triangle Park.
Construction of the Global Translational Research Institute, a 150,000 square-foot building projected to cost $70 million, could start as early as this fall, the Hamner chief executive told members of the Triangle Area Research Directors Council at their March 16 meeting.
The building is part of a $500 million expansion plan Greenlee unveiled in 2006. The plan envisions five buildings of labs and office space - a research hub focused on drug safety early in the development of new medicines.
Greenlee’s vision for the Hamner is inspired by biomedical research hot spots like the Salk Institute in San Diego, Calif., the Scripps Research Institute in La Jolla, Calif., and Jupiter, Fla., and the Broad Institute in Cambridge, Mass.
At the TARDC meeting, Greenlee showed a map of Cambridge, with the Broad Institute at the center of a triangle that had Harvard University, the Harvard Medical School and Massachusetts General Hospital as its corners. “This is an instructive model,” he said and pointed out that the Hamner sits in the middle of a similar node of knowledge with the University of North Carolina at Chapel Hill, Duke University and N.C. State University as the corners of the triangle.
“We don’t want to become Cambridge,” Greenlee said. “We want to create the energy of Cambridge.”
In the past five years, the Hamner has already made headway in pursuit of the ambitious expansion plan: A research partnership with UNC, research footholds in China and a collaboration with the Food and Drug Administration to reduce drug-induced liver injuries.
In June 2009, Janet Woodcock, head of the FDA’s Center for Drug Evaluation and Research, cut the ribbon at the opening of the Hamner’s Institute for Drug Safety Sciences, which built on the more than 30-year expertise the Hamner has with chemical toxins.
RTP panels address rogues gallery of multidrug-resistant bacteria
Tuesday, March 1, 2011, 2:29 pm No Comments | Post a CommentHow to prevent bacterial infections associated with poor hygiene in hospitals, nursing homes and day care centers has become a necessary though rarely pleasant topic for healthcare providers.
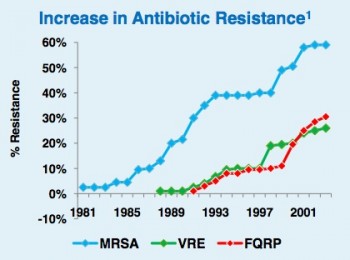
Every year, an estimated 5 percent of all hospitalized Americans, or about 1.7 million, are treated for a healthcare-associated infection. About 90,000 of them die, according to numbers reported by the Centers for Disease Control and Prevention. The infections are caused by multiple bacteria that can be traced back to healthcare settings and 14 percent involve a superbug, methicillin-resistant staphylococcus aureus or MRSA.
After rising rapidly in the 1990s, the number of MRSA cases began to decrease in the past decade, but following in MRSA’s footsteps are superbug wannabes such as floroquinolone-resistant pseudomonas aeruginosa (FQRP), vancomycin-resistant enterococci (VRE) and clostridium difficile, a bacterium that wreaks havoc after antibiotics wipe out healthy gut flora.
Efforts to reduce healthcare-associated infections received boosts in the past few years.
In 2008, the Centers for Medicare and Medicaid Services stopped paying hospitals for infections they considered “serious complications that should never occur in a hospital” and private health insurers began to follow suit. The following year, the federal stimulus bill provided states with about $50 million to establish surveillance and prevention programs.
North Carolina’s state plan to monitor and prevent healthcare-associated infections, which took effect in January and relies on voluntary reporting, is such a program.
“It’s not inevitable that you go into the [intensive care unit] and you get a [central line-associated] bloodstream infection,” said Dr. Megan Davies, chief of the N.C. Division of Public Health’s epidemiology section.
Davies was one of five infectious disease experts in the Research Triangle who addressed healthcare-associated infections and the rogues gallery of multi-drug resistant bacteria. The Feb. 22 panel discussion was put together by Duke University and Becton Dickinson, a New Jersey-based medical instruments company whose corporate innovation center is in Research Triangle Park.
Healthcare-associated infections add an estimated $28 billion to $33 billion in national healthcare costs every year, according to a report the CDC published in 2009.
Avoidable infections can enter the body at a surgical site or through a catheter, a ventilator or a central line used to supply medication, blood and fluids directly into the bloodstream.
In North Carolina, large programs to collect infection data and improve infection control have existed since 1997: the Statewide Program for Infection Control and Epidemiology, or SPICE, at the University of North Carolina School of Medicine and the Duke Infection Control Outreach Network, or DICON, that linked the Duke University School of Medicine and 39 community hospitals.
Central line-associated bloodstream infections and cases involving MRSA have decreased in the past decade due to efforts by SPICE and DICON.
But direct costs from dealing with healthcare-associated infections statewide are estimated to still exceed $280 million per year, according to the N.C. Department of Health and Human Services.
Innovations to prevent these infections such as special cleaning and medical supplies exist, said William Rutala, director of SPICE and one of the five infectious disease experts on the panel. But better compliance with more basic prevention tools such a hand hygiene would be an important first step.
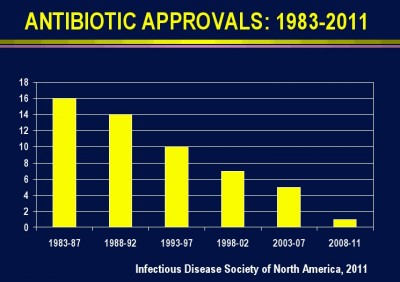 Only an average 40 percent of healthcare workers washed their hands in accordance with CDC guidelines, studies conducted in the 1990s showed. And other studies show that only about one-third of the surfaces at high risk of harboring infectious bacteria in hospital rooms were thoroughly cleaned before new patients came in, Rutala said.
Only an average 40 percent of healthcare workers washed their hands in accordance with CDC guidelines, studies conducted in the 1990s showed. And other studies show that only about one-third of the surfaces at high risk of harboring infectious bacteria in hospital rooms were thoroughly cleaned before new patients came in, Rutala said.
Fewer and fewer new antibiotics to battle the multi-drug resistant bacteria is yet another problem, said Dr. David Weber, associate chief of staff at UNC Health Care who was another infectious disease expert on the panel.
Years of antibiotic overuse and patients cutting short antibiotic treatments are driving forces behind the rogues gallery - not only in healthcare settings but maybe also in livestock farming.
About two-thirds of the MRSA central-line bloodstream infections in hospitals involve bacteria that came from outside the hospital but whose origin isn’t clear, according to Dr. Vance Fowler, an infectious disease specialist at Duke University.
Antibiotics are used extensively to promote growth in livestock farming, said Jorge Ferreira, a graduate student at the N.C. state University College of Veterinary Medicine. Daily use of antibiotics is also normal in dairy cows.
Fowler and Ferreira are collaborating on research to find out more about MRSA and whether the superbug is transmitted from animals to humans. They presented some of their findings as part of a panel discussion at the N.C. Biotechnology Center in RTP, a few hours after the infectious disease panel met in Durham.
So far, Ferreira reported, MRSA strains have been found in pigs, cows, dogs, cats and even hamsters.
Global health: What’s in it for the Research Triangle?
Wednesday, February 16, 2011, 5:25 pm No Comments | Post a CommentTravel can spread diseases as seafaring Europeans proved about 500 years ago, delivering smallpox, influenza and the bubonic plague to the Americas and in return bringing syphilis back with them to Europe.
So it shouldn’t come as a surprise that a biotech hot spot like North Carolina’s Research Triangle, where scientists are taking aim at diseases like HIV/AIDS, diabetes and cancer, is also a hub for global health research - an emerging academic discipline that has gained significance as international travel, trade and finance have picked up.
North Carolina’s global health sector supports at least 7,000 jobs, according to a Duke University study that was based on 2007 data and published last year. The sector generates more than $500 million in annual salaries and wages and more than $18 million in annual tax revenue. Most of the jobs are in the Triangle, home to three large universities, multiple research institutes and nonprofits dedicated to boost health and health care and hundreds of businesses involved in research and development.
The accumulation of brainpower makes the Research Triangle one of the few places in the U.S. where emerging diseases will be researched, medicines to treat them will be developed and programs to improve people’s wellbeing at home and abroad will be established.
“Global health involves highly interdisciplinary and interconnected areas that include human and animal health, medicine, law, engineering, economics, environmental science, agriculture and the social and biological sciences,” as four Duke researchers write in the North Carolina Medical Journal’s latest issue.
Their point of view is part of the NCMJ’s global health forum, which takes up much of the issue.
More than two dozen contributors, including nurses, doctors, community advocates, economists, a veterinarian, a lawyer and a pharmacist, explore what role North Carolina health care professionals and institutions play in global health and the benefits the state is reaping in return.
The forum’s premise follows much the same lessons we learned from the seafaring Europeans: Global health oftentimes is local health.
Today, HIV/AIDS has replaced the bubonic plague. Air travel spreads new influenza strains like H1N1. An obesity epidemic is threatening a rise in diabetes worldwide. Rising temperatures, an effect of global warming, are changing not only growing conditions for plants but also living conditions for animals that carry diseases.
North Carolina is feeling the effects of all these global developments:
- The number of people living with HIV/AIDS in North Carolina and in the Raleigh-Cary area is higher than the national average, according to the U.S. Centers for Disease Control and Prevention.
- Children ages 10 to 17 in North Carolina are among the most obese in the U.S., according to a 2009 report of the N.C. Department of Health and Human Services.
- Chronic disease and infant mortality rates in some eastern North Carolina are comparable to those in developing countries such as Malaysia, Thailand and Nicaragua, according to figures of the N.C. State Center for Health Statistics. The eastern part of the state also faces a particular shortage of health workers.
- North Carolina is getting warmer from the beaches through the Piedmont and across the mountains, according to the Arbor Day Foundation. Since 1990, much of North Carolina has switched from a zone where plants must survive temperatures as low as 0 degrees Fahrenheit to a zone where temperatures don’t dip below 10 degrees Fahrenheit. North Carolina has a long history of tick-borne diseases and research has shown milder winters increase tick-borne encephalitis among humans.
But North Carolina also stands to benefit from the work done in the Research Triangle to address global health issues:
- Researchers at the University of North Carolina at Chapel Hill and Family Health International, a Durham nonprofit, helped test a vaginal gel that contained 1 percent of the Gilead HIV/AIDS drug tenofovir. The test involved South African women and demonstrated that the gel reduced the risk of an HIV infection by up to 59 percent, according to results first published last year.
- RTI International, a research institute in Research Triangle Park, has developed a behavioral program to reduce the likelihood that at-risk women will get infected with HIV. The program is recognized by the CDC and implemented globally and locally.
- The UNC-CH chapter of Engineers without Borders has been involved in improving water quality in communities in Eastern Europe, Latin America and just outside Chapel Hill. Tests in a historically black neighborhood that borders the Orange County landfill showed that nine of 11 wells did not meet federal water quality standards.
- In 2009, UNC and CDC started a program in eastern North Carolina that used global models of mircofinance. It helps women start in business and provides health education.
- Nurses, physicians and dentists educated in India, the Philippines, Nigeria and Columbia are easing the health worker shortage in North Carolina. In the Research Triangle, about 15 percent percent of the physicians, 5.8 percent of nurses and less than 1 percent of dentists were educated outside of the U.S., according to an analysis by a postdoctoral fellow in the UNC School of Nursing that was based on unpublished data from the 2008 North Carolina Professions Data System.
Read all of the contributions to the NCMJ’s global health forum here.
Read here why in 2009 the Research Triangle was the first stop in the U.S. global health revamp.
To rein in dengue fever, researchers go after the virus and mosquitoes
Thursday, February 3, 2011, 12:29 am No Comments | Post a CommentThe high-pitched hum of a mosquito increasingly carries the threat of disease in many parts of the world.
Mosquitoes can transmit West Nile, malaria, yellow fever, chikungunya and other viral diseases when they bite. The infections kill more than 1 million people every year.
Researchers in North Carolina’s Research Triangle are working on stemming the spread of mosquito-borne diseases, particularly dengue fever.
Globalization and poorly planned urbanization has increased the number of dengue infections more than four-fold since 1970s, putting two-fifths of the world population at risk, according to the World Health Organization. Along with the spread of the virus to about 60 countries, the risk of hemmorrhagic dengue fever has gone up. The severe form of the disease has become a leading cause of hospitalization and death among children in Southeast Asia.
“Dengue is a huge problem in the tropics,” said Aravinda de Silva, assistant professor of microbiology and epidemiology at the University of North Carolina at Chapel Hill.
U.S. travelers to Southeast Asia, Latin America and Africa can get infected - four cases of dengue fever were reported in North Carolina last summer - but local mosquitoes rarely pass on the virus outside of Hawaii and the Florida Keys.
De Silva spoke Tuesday at a forum on emerging infectious diseases at the N.C. Biotechnology Center. Other speakers were Katia Koelle, assistant professor of biology at Duke University, and Fred Gould, professor of agriculture at N.C. State University. The three talked about research under way to prevent dengue and possibly other mosquito-borne diseases. Read more…
Epidemiologist tracks environmental clues linked to rising autism rates
Tuesday, December 7, 2010, 9:25 pm 1 Comment | Post a CommentIrva Hertz-Picciotto is a slight woman stepping squarely into a brawl: the controversy over rising autism rates.
That the rates have been rising is undisputed. In the 1980s, about 6 of 10,000 were believed to have an autistic disorder, according to a 2007 paper. Today, autism spectrum disorders affect about 40 in 10,000. That’s a 600 percent increase, but opinions differ over what’s causing the increase.
Many researchers see forms of autism as predominantly inherited disorders whose diagnoses have dramatically increased, because parents have become more aware of telltale signs and children get diagnosed earlier, more frequently and with less severe symptoms than 30 years ago.
Others like Hertz-Picciotto, a professor of public health sciences at the University of California at Davis, aren’t so sure genes are the only culprits. But lacking data, they have had little to go on beyond questioning inconsistencies. How, for example, can it be that one identical twin has an autistic disorder but the other doesn’t, even though they share the same genetic information? Read more…
Visiting Second Life to see the 3D AIDS quilt
Friday, December 3, 2010, 1:18 am No Comments | Post a CommentThe launch of the three-dimensional quilt during World AIDS Day Wednesday was accompanied by, as you would expect, songs, images and poems to remember loved ones who lived with and died from HIV.
But in every other respect this gathering was different from the largest community arts project in the world, the AIDS Memorial Quilt that was founded in 1987.
The 3D AIDS quilt, which includes contributions from the University of North Carolina at Chapel Hill Center for AIDS Research and the Triangle Global Health Consortium, is laid out below an enormous tree that grows on Storybook Island in Second Life, a three-dimensional virtual world maintained by Linden Lab of San Francisco.
As Jena Ball, one of the creators of the 3D AIDS quilt, put it, this quilt “doesn’t have to be folded and stored. It’s available 24/7, can live in multiple places and grow to any size.”
Ball, a writer who recently moved from Los Angeles to North Carolina’s Research Triangle area, made that point through her avatar, Jenaia Morane, during the launch celebration, which took place in an auditorium inside the tree on Storybook Island. Because, you see, you can only visit the 3D quilt in the form of an avatar. I was there as Zaidy Xenga, a redhead wearing a gray suit and one black shoe.
With the 3D AIDS quilt, Ball and her collaborators at Startled Cat studios - Martin Keltz, an Emmy award winning producer, and Doug Thompson, an Internet marketing entrepreneur - built on the Karuna initiative, a HIV/AIDS storytelling project in Second Life that kicked off in 2008 with a grant from the National Library of Medicine.
The initiative now consists of multiple Second Life islands, all owned by Startled Cat. On Karuna island, avatars can, for example, read the panels in the AIDS poetry garden, learn about the human immunodeficiency virus or visit the Ryan White tree. The seven-part Uncle D story quest is spread out over six islands. Avatars going on the quest can visit the house of Uncle D, a person who lived with HIV, and read his diary.
Here’s a video of Keltz’s avatar, Marty Snowpaw, going on one of the Uncle D story quests:

The 3D AIDS quilt is on yet another Second Life island. The quilt consists of rooms that commemorate people who have died of AIDS. My avatar, Zaidy Xenga, teleported to a few of the rooms.
One of the rooms is dedicated to Bobby, who loved flying. My avatar arrived in the room and looked at a single-engine plane frozen in mid-flight.
The next visit took me into the sleeping quarters of an AIDS orphanage in South Africa. The beds were made of logs. Spread across the floor was a play carpet that had the streets and buildings of a village woven into it. A slide show on one wall showed pictures of South African children playing.
The room is a contribution of the Triangle Global Health Consortium and represents a memory of Nicole Fouche, TGHC’s executive director who grew up in South Africa. The memory is of a day in a park when a child took Fouche’s hand. The incident led her to realize there were entire orphanages in South Africa filled with children who lost their parents to AIDS, Fouche’s avatar said during the launch ceremonies.
Banners above the beds displayed the names of TGHC’s members, including Glaxo SmithKline, at whose U.S. headquarters in RTP the first AIDS drug was discovered in 1984, Duke University, UNC and RTI International.
The TGHC room on the 3D quilt commemorates the more than 16 million children under 18 who have been orphaned by HIV worldwide.
As Zaidy Xenga I also visited the room contributed by the UNC Center of AIDS Research, which is a collaboration of UNC, RTI and Family Health International.
On panels on the room’s wall, Vanessa White, aka Vanie MacBeth in Second Life, tells the story of Ann, who volunteered to speak about living with HIV to more than 300 UNC students on World AIDS Days. White manages the community outreach for the UNC Center for AIDS Research and recruited Ann before she died at 42 of complications from AIDS. An empty chair below the last story panel represents her death.
My avatar also sat next to avatars of more than 40 other visitors from across the world who gathered in the auditorium inside the tree on Storybook Island. Some wore billowing dresses, other jeans, wings or Werewolf skins. In Second Life, you can take on any shape you like, even glowing green skin. One of the avatars had “I am HIV+” written as part of its name.
On the panel in the center of the auditorium sat Jokay Wollongong, the avatar of Jo Kay, an Australian woman who created the JokaydiaGrid, a virtual world for educators and students age 10 to 16. A copy of the 3D AIDS quilt on JokaydiaGrid is available for commemorative rooms build by pre-teens and teens who are not allowed to go onto Second Life.
North Carolina’s medical device industry faces strong headwinds
Wednesday, December 1, 2010, 11:17 pm 1 Comment | Post a CommentStrengthening the emerging medical device industry in North Carolina, a state better known as a biotech hub, is a no-brainer no longer.
Sure, North Carolina’s universities are still brimming with ideas, students to test new technologies in a lab and professors to lend their expertise to startup companies, especially in the Research Triangle Park area, home to biomedical engineering departments at Duke University, the University of North Carolina at Chapel Hill and N.C. State University and two teaching hospitals.
But raising cash to pay for development has become more difficult in the past two years, according to two venture capitalists and an investment banker who addressed the challenges facing medical device companies Tuesday at North Carolina’s third Medtech conference, which took place in Durham.
Regulatory scrutiny and cost-saving pressures at hospitals have also increased, according to Ernst & Young’s medical technology report 2010.
The medical device business used to be a haven of gadget geekdom, “focused on the newness, the sexiness” of the latest technology, said Mike Constantino, Southeast area life sciences industry leader at Ernst & Young’s office in Raleigh. “Whether patients were getting better was secondary.”
Now, being new is no longer enough. The technology must increase efficiency and improve health outcomes.
Overall, the U.S. medical device industry has fared better than most other industries during the recession, according to Ernst & Young’s report.
Large companies have access to plenty of capital. For example, AGA Medical, a Minneapolis device maker with nearly $200 million in annual sales, raised $94.4 million in an initial public offering a year ago.
But the situation is different for companies with less than $50 million in annual revenue or startups relying on investors to develop a product and bring it to market. That’s the industry segment where many North Carolina device makers fit.
The state’s medical device industry consists of close to 400 companies, according to Ibility, an industry organization that was founded last year with the help of $2.5 million in state funding. A listing of about 250 of them shows that at least 40 percent of them have 20 or fewer employees.
About one-third of North Carolina’s 400 medical device companies have operations in the RTP area, including startups like Physcient, companies with products on the market like Bioptigen and Metabolon and publicly traded companies like New Jersey-based BD.
BD, which generates more than $7 billion in annual sales, this year finished a $12.7 million renovation of its technology and innovation center in RTP, opened a $14 million manufacturing facility west of Durham and announced plans to build a distribution center southeast of Raleigh. (Read about BD’s expansion in North Carolina here.)
With fewer than 20 employees and less than $5 million in annual revenue each, Metabolon and Bioptigen have to rely on venture capital and other private investors to develop new products and get regulatory approval to sell them.
Metabolon‘s latest product is a biomarker test that identifies people at high risk for diabetes. Bioptigen has developed scanners that map the back of the eye in microscopic detail and allow surgeons to identify diseases at early stages.
Physcient, a three-year-old startup, is working on its first product, an surgical tool that opens the rib cage for heart and lung surgeries. The tool, which can be operated electronically with a smart phone, inflicts less damage to tissue and bone than mechanical thoracic retractors that have been used in hospitals for more than 70 years.
Private investors are key to keep the lights on and the development going at Physcient.
All medical device companies, regardless of size, have to deal with more stringent regulatory scrutiny, which add time and costs to the approval process, as well as cost-savings pressures at hospitals and a new 2.3 percent excise tax on medical device sales that takes effect 2013, both results of health care reform. But small companies and startups face an additional challenge: A crunch in venture capital investments, particularly in early-stage rounds.
In 2009, medical device companies raised less than $3 billion in venture capital in the U.S., according to the Ernst & Young report. Only 13 percent of the rounds were early-stage, the least since 2001.
North Carolina was absent from the map of U.S. regions that led in funds raised by medical device companies, even though one company, Durham-based TransEnterix, made the top 10 venture rounds list with a $55 million fundraiser completed in October 2009.
Short and round and poor
Tuesday, November 23, 2010, 2:48 pm 1 Comment | Post a CommentWaist lines are expanding across the world, not just in the U.S., one of the countries leading the worldwide obesity epidemic. But while the additional calories are also boosting the average height of people in Asia and Latin America, Americans are becoming rounder and shorter.
What seems like a statistical error - considering too little, not too much, food tends to stunt growth - isn’t, according to John Komlos, an economist and professor at the University of Munich, who taught and researched at Duke University in the 1980s. He is currently a fellow at the National Humanities Center in Research Triangle Park.
“Within half a century a veritable metamorphosis in the shape of the American population took place without notice: from being the tallest in the world still around World War II, Americans have become one of the most obese at the onset of the 21st century,” Komlos wrote in a discussion paper that was published in 2003.
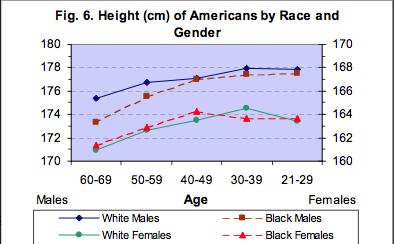
The average height of Americans rose about 2 inches in the past 150 years while the Dutch, for example, grew about 6 inches taller. In the past 20 to 30 years, American women and white American men actually shrunk a bit.
Komlos presented his research at the National Humanities Center a week before Thanksgiving, at the end of the same day that had started next door, at the N.C. Biotechnology Center, with a presentation by Barry Popkin, a professor at the University of North Carolina at Chapel Hill and the author of “The World is Fat.”
Komlos and Popkin are both trained economists, but the data they collect - Komlos on height and Popkin on weight - focus on human well-being rather than on a country’s output of goods and services. In the process, both redefine economics at a time when technology and cheap, processed foods are replacing physical labor and traditional diets worldwide.
Popkin is particularly alarmed by how quickly countries like China and Mexico are catching up and getting fatter. What has taken the U.S. about a century, happened in the past two to three decades in Asia and Latin America.
“It’s going fast, fast, fast,” Popkin said at the breakfast meeting of the Triangle Global Health Consortium. And similarly to the U.S., he added, the resulting burden of disease - diabetes, hypertension and heart disease - is shifting towards the poor.
Their research, which touches on disciplines as diverse as genetics and history, has come up with some surprising findings. But each researcher takes a different approach to what should be done to improve health and lower the burden of disease around the globe.
Komlos has scoured archives for more than a quarter century to collect hundreds of thousands of historic height measurements from military recruits, passport applicants, runaway slaves and indentured servants. (Read a feature in The New Yorker about his research here.)
The large data sets revealed trends that go beyond genetics and reflect the influence nutrition, medical care, education and family status and income can have on children and therefore on the well-being of entire population segments once those children become adults. Komlos called this approach “humanistic economics.”
“Height is important, because childhood health has a long reach into the rest of the life,” he said.
During the period before the Civil War, white Southerners were the tallest population segment in the U.S. because they had good access to food, Komlos found by looking at height records of Georgia prison convicts. At the same time, heights declined across Europe as people left the countryside and farming and moved to the cities to find jobs in the factories.
The Oliver Twists of industrializing England in the first half of the 19th century averaged 5-feet-1-inch at 18, Komlos said. Their contemporaries in the British gentry grew 9 inches taller on average.
By the end of the 19th century, Americans were the tallest, but average U.S. height stagnated as technological innovations such as cars, radios, television and computers boosted the U.S. gross national product during the 20th century.
At the same time, Americans started to gain weight. On average, Citadel military cadets are more than 25 pounds heavier today than they were after World War I, Komlos found.
And then, there’s the report card on child well-being in 21 rich countries that UNICEF published in 2007. The report card ranked the U.S. second to last. The Netherlands, home of the tallest people, came in first.
To close the height gap that is opening up in the U.S., Komlos suggested to bolster the social safety net, particularly prenatal care, and the access to nutritious food.
Popkin supports an approach that’s more grassroots and includes consumer education, particularly about caloric beverages that are loaded with sugar, and public health advocacy for healthier food options in schools, churches and at the workplace.
Already, more than 1 billion people worldwide are overweight or obese, according to figures by the World Health Organization. Every year, 10 million more join the group, Popkin said. A shift in how the world eats, drinks and moves is the reason, he said.
Fruits, vegetables and beans are being increasingly replaced by meats, dairy and processed, energy-dense but nutrient-poor, cheap foods that are available in supermarkets around the world.
More than half of these processed foods in supermarkets are made locally, not by the 10 to 15 largest multinational food companies, Popkin said. “Kraft, Nestle, Unilever are just the tip of the iceberg.”
The result? French fries are named by U.S. parents as the first vegetable to which they introduced their 7-month-olds. About one-third of Americans don’t know how to cook. The number of overweight children in the U.S. has doubled in the past 30 years. In North Carolina, about one-third of the children are overweight or obese.
And countries such as Mexico, China and India are catching up quickly. About two-thirds of Mexicans and one-third of Chinese are overweight or obese.
What’s worse, Popkin pointed out, populations who are getting fat and fatter quickly after centuries of malnutrition are more prone to develop diabetes, hypertension and heart diseases than Americans and Europeans.