Posts Tagged ‘Duke’
Humans, monkeys age the same, say Duke primatologists
Sunday, March 27, 2011, 7:13 pm No Comments | Post a CommentOriginally published: 3/17/11
Humans share 98 percent of their DNA with monkeys. Clearly, the two species have a few things in common. One, say researchers from Duke University, is how we age.
Dr. Susan Alberts, a Duke biology professor, has been studying baboons in Kenya’s Amboseli National Park for quite some time. In fact, she’d just gotten off a flight home, she mentioned when interviewed.
Alberts is one of several Duke scientists who have teamed up with universities across the world to study aging behavior in wild primates. She said data was combined from seven different studies on non-human primates, each spanning 25 to 50 years. Two of these—the Jane Goodall Institute study on chimpanzees and Alberts’s Amboseli study on baboons—were based at Duke.
Findings from the studies appear in the March 11 edition of Science.
The studies chronicle primates over the course of their lives. Monkey populations were observed for births, deaths and physical deterioration. Alberts said long-term primate studies like these are invaluable to putting the human experience in perspective.
“Before, we didn’t have anything to compare to that was like us,” Alberts said. “So we were comparing ourselves to lab mice. And we are really different than lab mice.”
Dr. William Morris, a Duke ecology and population biology professor who assisted Alberts, said main conclusion of the report was that aging patterns and mortality risks coincide between humans and non-human primates.
“Your chance of dying increases with age in a similar way whether you’re a gorilla or a baboon or a human,” said Morris. “Humans still win, but we’re not too far away from our primate relatives.”
According to the report, female chimpanzees often live into their forties, some even into their fifties. Males live into their thirties but are mostly dead by their early forties. Morris said the monkey with the longest life expectancy was not the chimp or gorilla, but rather the lesser-known Brazilian muriqui, which can survive all the way into its seventies.
That is not too far off from the average life expectancy of a human, said Dr. Anne Pusey, chair of Duke’s evolutionary anthropology department. Nowadays, the typical American male will live into his eighties. Females, she said, live slightly longer. The gender difference is more pronounced in monkeys, though, because of male-male competition for reproductive opportunities with a limited number of females.
Pusey has been working with renowned British primatologist Jane Goodall at her chimpanzee park in Tanzania since 1970. In the wealth of data she’s collected over four decades, she has developed an eye for identifying chimp aging behavior.
“Just knowing more about mortality patterns in other species helps us think about the evolution of our mortality patterns and understand which patterns are fixed and which are more elastic,” Pusey said. In the future, she and her colleagues plan to investigate how reproductive rates change with age.
“Humans are unusual in this regard because we hit menopause and continue to live a long time afterwards,” she said. “But female chimps go on having babies up until they die.”
Pusey took on her job at Duke last year. She said she was attracted to the area because she feels it’s one of the best of its kind in the country. Also, she had heard about Dr. Alberts’ study and discovered how much potential there is for primate research in the Triangle region.
Alberts said she’s interested in how animals use social behavior to solve environmental problems and how that impacts their survival. What characterizes the human race, she said, is that we’re primarily monogamous, which levels out competition among males.
This might seem counterintuitive at first. If females only mate with one male, wouldn’t there be increased drive for men to settle down with the most desirable female? Alberts said it is actually a great equalizer for the men, and everyone still ends up with a partner.
However, in non-human primate species, not everyone does. The females mate with multiple fathers, but not every male passes that litmus test.
“If females only mate with one male, it isn’t how many kids he’s going to have but how good a mate he’s going to get,” she said. “In primates, the least successful male wouldn’t have any kids at all.”
One finding that surprised her was that primate males are able to differentiate their own offspring. She found this remarkable since females mate with many different males in the course of a lifetime and there’s no discernable way for fathers to keep track of who’s whose. Paternal care goes very deep in our primate roots, she said.
“Human males are very good fathers, especially compared to most mammals,” said Alberts.
So in a lot of ways, socialization has factored into reproduction and life expectancy. Insight like this, Morris said, paves the way to understanding how human evolution has digressed from that our hairy ancestors.
“We live longer than the other primates because of the environment we create for ourselves,” he said. “Nutrition, modern medicine, health care—other primates don’t have these things.”
To Morris, the importance of the Amboseli study is in advocating long-term primate research because he thinks that’s how we really learn about the aging process. He said it’s much different than the plants he studies.
“With trees you can take a look at the core and see how old it is,” Morris said.
“You can’t do that with baboons and monkeys. You really need to follow them around to get the whole picture.”
One man’s vision of affordable health care for all
Monday, March 14, 2011, 3:17 pm No Comments | Post a CommentDurham is home to Duke University hospital, rated one of the best 50 hospitals in the U.S., but Durham also has one of the highest HIV infection rates in North Carolina. Sixty-five percent of adults are overweight or obese and an estimated 15 percent of the children in Durham are uninsured, according to the 2010 State of the County health report.
Considering that the Duke University Health System dominates healthcare in Durham, the community’s health status stands in stark contrast to the hospital’s nationwide ranking. Dr. Victor Dzau, Duke’s chancellor for health affairs and chief executive of Duke University Health System, acknowledged as much during a speech he gave March 9 at the Research Triangle Park Rotary Club’s Luther Hodges Ethics Luncheon.
But then Durham is no exception. Communities surrounding the best health systems in the country often have the worst health status, Dzau said.
The problems these communities face with access to healthcare and healthcare quality and affordability in many ways epitomize national challenges: Healthcare spending has increased faster than the economy and now represents 16 percent to 17 percent of the U.S. gross national product, but the U.S. population isn’t getting healthier. Obesity and diabetes rates are up, the infant mortality rate is higher in the U.S. than in most other developed countries and about 50 million American age 18 to 64 are uninsured, according to the Centers for Disease Control and Prevention.
“Some people say we’re in a crisis,” Dzau said.
As a doctor who promised to hold service above self and as the head of a health system whose costs for services to patients unable to pay reportedly increased from $45 million in fiscal year 2009 to $47.7 million in fiscal year 2010, Dzau said he believes healthcare is a human right and he worries about who’s going to pay for it.
He sees part of the solution in the federal healthcare reform act that passed last year. The law “has lots of elements we should embrace,” Dzau told RTP Rotarians, even though it’s “pretty scary for providers. It changes my entire business model.”
But he also envisions a role for academic health sciences centers like Duke to better pass on their knowledge from the bench to the bedside and to help surrounding communities come up with strategies for prevention and treatment. (More about organizational changes at Duke to embrace Dzau’s vision here.)
Implementing the reform act, which would expand health insurance to more than 30 million uninsured Americans, is projected to cost more than $1 trillion over nine years, according to a Congressional Budget Office report. But it also promises to change an inefficient and expensive fee-for-service system in which healthcare providers are paid whether treatments work or not.
Another CBO report estimated that by 2019 reform act provisions will reduce the national deficit by up to $143 billion.
Healthcare reform aims to, for example, reduce the more than $28 billion spent every year on infections by bacteria that can be traced back to healthcare settings. Provisions in the reform act include programs to increase measuring and reporting of healthcare-associated infections, to restrict reimbursements to hospitals for HAIs and to establish financial penalties for providers with high HAI rates. (More about efforts to reduce HAIs in North Carolina hospitals here.)
Other provisions restrict reimbursements to hospitals that discharge patients too quickly and have to readmit them within 30 days of the discharge.
The reform act would also test whether healthcare costs can be reduced by bundling payments to multiple providers, from the physician who treats, say a patient being admitted for a heart attack, to the home-health nurse who makes sure the patient takes his medicines, adjusts his diet and sticks with an appropriate exercise regimen.
“It’s going to be painful,” Dzau said. But “we’ve got to get the cost down and keep the quality.”
Financially, the status quo of U.S. healthcare is no longer tenable, he said.
Private health insurers have ratcheted up copays and deductibles for years to corral payments. To deal with a drop in tax revenue and a rise in Medicaid enrollments, states have begun slashing Medicaid programs to fill budget deficits. Meanwhile, hospitals have been shifting costs from Medicare and Medicaid patients to privately insured patients to reduce losses, Dzau said.
In addition to charity care for patients who couldn’t pay, Duke reported it absorbed $62 million in losses during fiscal year 2010 because Medicaid reimburses only 60 cents for every $1 spent on patients.
RTP panels address rogues gallery of multidrug-resistant bacteria
Tuesday, March 1, 2011, 2:29 pm No Comments | Post a CommentHow to prevent bacterial infections associated with poor hygiene in hospitals, nursing homes and day care centers has become a necessary though rarely pleasant topic for healthcare providers.
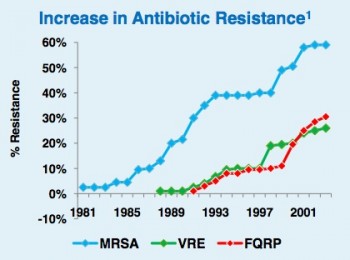
Every year, an estimated 5 percent of all hospitalized Americans, or about 1.7 million, are treated for a healthcare-associated infection. About 90,000 of them die, according to numbers reported by the Centers for Disease Control and Prevention. The infections are caused by multiple bacteria that can be traced back to healthcare settings and 14 percent involve a superbug, methicillin-resistant staphylococcus aureus or MRSA.
After rising rapidly in the 1990s, the number of MRSA cases began to decrease in the past decade, but following in MRSA’s footsteps are superbug wannabes such as floroquinolone-resistant pseudomonas aeruginosa (FQRP), vancomycin-resistant enterococci (VRE) and clostridium difficile, a bacterium that wreaks havoc after antibiotics wipe out healthy gut flora.
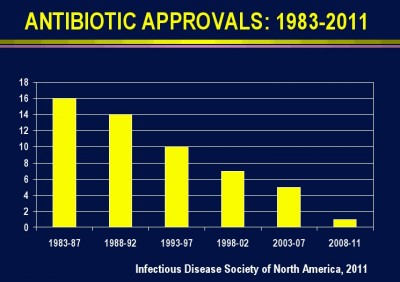
Efforts to reduce healthcare-associated infections received boosts in the past few years.
In 2008, the Centers for Medicare and Medicaid Services stopped paying hospitals for infections they considered “serious complications that should never occur in a hospital” and private health insurers began to follow suit. The following year, the federal stimulus bill provided states with about $50 million to establish surveillance and prevention programs.
North Carolina’s state plan to monitor and prevent healthcare-associated infections, which took effect in January and relies on voluntary reporting, is such a program.
“It’s not inevitable that you go into the [intensive care unit] and you get a [central line-associated] bloodstream infection,” said Dr. Megan Davies, chief of the N.C. Division of Public Health’s epidemiology section.
Davies was one of five infectious disease experts in the Research Triangle who addressed healthcare-associated infections and the rogues gallery of multi-drug resistant bacteria. The Feb. 22 panel discussion was put together by Duke University and Becton Dickinson, a New Jersey-based medical instruments company whose corporate innovation center is in Research Triangle Park.
Healthcare-associated infections add an estimated $28 billion to $33 billion in national healthcare costs every year, according to a report the CDC published in 2009.
Avoidable infections can enter the body at a surgical site or through a catheter, a ventilator or a central line used to supply medication, blood and fluids directly into the bloodstream.
In North Carolina, large programs to collect infection data and improve infection control have existed since 1997: the Statewide Program for Infection Control and Epidemiology, or SPICE, at the University of North Carolina School of Medicine and the Duke Infection Control Outreach Network, or DICON, that linked the Duke University School of Medicine and 39 community hospitals.
Central line-associated bloodstream infections and cases involving MRSA have decreased in the past decade due to efforts by SPICE and DICON.
But direct costs from dealing with healthcare-associated infections statewide are estimated to still exceed $280 million per year, according to the N.C. Department of Health and Human Services.
Innovations to prevent these infections such as special cleaning and medical supplies exist, said William Rutala, director of SPICE and one of the five infectious disease experts on the panel. But better compliance with more basic prevention tools such a hand hygiene would be an important first step.
 Only an average 40 percent of healthcare workers washed their hands in accordance with CDC guidelines, studies conducted in the 1990s showed. And other studies show that only about one-third of the surfaces at high risk of harboring infectious bacteria in hospital rooms were thoroughly cleaned before new patients came in, Rutala said.
Only an average 40 percent of healthcare workers washed their hands in accordance with CDC guidelines, studies conducted in the 1990s showed. And other studies show that only about one-third of the surfaces at high risk of harboring infectious bacteria in hospital rooms were thoroughly cleaned before new patients came in, Rutala said.
Fewer and fewer new antibiotics to battle the multi-drug resistant bacteria is yet another problem, said Dr. David Weber, associate chief of staff at UNC Health Care who was another infectious disease expert on the panel.
Years of antibiotic overuse and patients cutting short antibiotic treatments are driving forces behind the rogues gallery - not only in healthcare settings but maybe also in livestock farming.
About two-thirds of the MRSA central-line bloodstream infections in hospitals involve bacteria that came from outside the hospital but whose origin isn’t clear, according to Dr. Vance Fowler, an infectious disease specialist at Duke University.
Antibiotics are used extensively to promote growth in livestock farming, said Jorge Ferreira, a graduate student at the N.C. state University College of Veterinary Medicine. Daily use of antibiotics is also normal in dairy cows.
Fowler and Ferreira are collaborating on research to find out more about MRSA and whether the superbug is transmitted from animals to humans. They presented some of their findings as part of a panel discussion at the N.C. Biotechnology Center in RTP, a few hours after the infectious disease panel met in Durham.
So far, Ferreira reported, MRSA strains have been found in pigs, cows, dogs, cats and even hamsters.
Triangle gaming hits the airwaves
Friday, February 25, 2011, 1:15 pm 2 Comments | Post a Comment I had a great opportunity a few weeks ago to discuss gaming in the Triangle with Chris Perrien on WXDU, Duke University’s noncommercial radio station (Chris also runs Blue Pane Studio, which created this blog).
I had a great opportunity a few weeks ago to discuss gaming in the Triangle with Chris Perrien on WXDU, Duke University’s noncommercial radio station (Chris also runs Blue Pane Studio, which created this blog).
His show on Feb. 13, aptly named Science in the Triangle, was the first in a series of interviews he’ll be doing on science and technology in Research Triangle Park.
This has been an exciting field to cover over the last year or so, and I’ve definitely learned a lot about why the Triangle area is the gaming’s industry’s No. 2 spot for production. More than 40 companies and 1,000 employees calling the area home.
Check out the interview in three parts here:
Audio clip: Adobe Flash Player (version 9 or above) is required to play this audio clip. Download the latest version here. You also need to have JavaScript enabled in your browser.
Audio clip: Adobe Flash Player (version 9 or above) is required to play this audio clip. Download the latest version here. You also need to have JavaScript enabled in your browser.
Audio clip: Adobe Flash Player (version 9 or above) is required to play this audio clip. Download the latest version here. You also need to have JavaScript enabled in your browser.
You can also subscribe to WXDU’s podcasts on iTunes.
I mentioned a few resources for people looking to get into the local game industry, including the Triangle Game Initiative. You can also find more information for the upcoming East Coast Game Conference, which runs April 13-14 at the Raleigh Convention Center. For job-seekers, there’s also the International Game Developers Association, a nonprofit professional organization with a Triangle chapter.
Know of more resources for discovering gaming in the Triangle? Add your thoughts in the comments!
Global health: What’s in it for the Research Triangle?
Wednesday, February 16, 2011, 5:25 pm No Comments | Post a CommentTravel can spread diseases as seafaring Europeans proved about 500 years ago, delivering smallpox, influenza and the bubonic plague to the Americas and in return bringing syphilis back with them to Europe.
So it shouldn’t come as a surprise that a biotech hot spot like North Carolina’s Research Triangle, where scientists are taking aim at diseases like HIV/AIDS, diabetes and cancer, is also a hub for global health research - an emerging academic discipline that has gained significance as international travel, trade and finance have picked up.
North Carolina’s global health sector supports at least 7,000 jobs, according to a Duke University study that was based on 2007 data and published last year. The sector generates more than $500 million in annual salaries and wages and more than $18 million in annual tax revenue. Most of the jobs are in the Triangle, home to three large universities, multiple research institutes and nonprofits dedicated to boost health and health care and hundreds of businesses involved in research and development.
The accumulation of brainpower makes the Research Triangle one of the few places in the U.S. where emerging diseases will be researched, medicines to treat them will be developed and programs to improve people’s wellbeing at home and abroad will be established.
“Global health involves highly interdisciplinary and interconnected areas that include human and animal health, medicine, law, engineering, economics, environmental science, agriculture and the social and biological sciences,” as four Duke researchers write in the North Carolina Medical Journal’s latest issue.
Their point of view is part of the NCMJ’s global health forum, which takes up much of the issue.
More than two dozen contributors, including nurses, doctors, community advocates, economists, a veterinarian, a lawyer and a pharmacist, explore what role North Carolina health care professionals and institutions play in global health and the benefits the state is reaping in return.
The forum’s premise follows much the same lessons we learned from the seafaring Europeans: Global health oftentimes is local health.
Today, HIV/AIDS has replaced the bubonic plague. Air travel spreads new influenza strains like H1N1. An obesity epidemic is threatening a rise in diabetes worldwide. Rising temperatures, an effect of global warming, are changing not only growing conditions for plants but also living conditions for animals that carry diseases.
North Carolina is feeling the effects of all these global developments:
- The number of people living with HIV/AIDS in North Carolina and in the Raleigh-Cary area is higher than the national average, according to the U.S. Centers for Disease Control and Prevention.
- Children ages 10 to 17 in North Carolina are among the most obese in the U.S., according to a 2009 report of the N.C. Department of Health and Human Services.
- Chronic disease and infant mortality rates in some eastern North Carolina are comparable to those in developing countries such as Malaysia, Thailand and Nicaragua, according to figures of the N.C. State Center for Health Statistics. The eastern part of the state also faces a particular shortage of health workers.
- North Carolina is getting warmer from the beaches through the Piedmont and across the mountains, according to the Arbor Day Foundation. Since 1990, much of North Carolina has switched from a zone where plants must survive temperatures as low as 0 degrees Fahrenheit to a zone where temperatures don’t dip below 10 degrees Fahrenheit. North Carolina has a long history of tick-borne diseases and research has shown milder winters increase tick-borne encephalitis among humans.
But North Carolina also stands to benefit from the work done in the Research Triangle to address global health issues:
- Researchers at the University of North Carolina at Chapel Hill and Family Health International, a Durham nonprofit, helped test a vaginal gel that contained 1 percent of the Gilead HIV/AIDS drug tenofovir. The test involved South African women and demonstrated that the gel reduced the risk of an HIV infection by up to 59 percent, according to results first published last year.
- RTI International, a research institute in Research Triangle Park, has developed a behavioral program to reduce the likelihood that at-risk women will get infected with HIV. The program is recognized by the CDC and implemented globally and locally.
- The UNC-CH chapter of Engineers without Borders has been involved in improving water quality in communities in Eastern Europe, Latin America and just outside Chapel Hill. Tests in a historically black neighborhood that borders the Orange County landfill showed that nine of 11 wells did not meet federal water quality standards.
- In 2009, UNC and CDC started a program in eastern North Carolina that used global models of mircofinance. It helps women start in business and provides health education.
- Nurses, physicians and dentists educated in India, the Philippines, Nigeria and Columbia are easing the health worker shortage in North Carolina. In the Research Triangle, about 15 percent percent of the physicians, 5.8 percent of nurses and less than 1 percent of dentists were educated outside of the U.S., according to an analysis by a postdoctoral fellow in the UNC School of Nursing that was based on unpublished data from the 2008 North Carolina Professions Data System.
Read all of the contributions to the NCMJ’s global health forum here.
Read here why in 2009 the Research Triangle was the first stop in the U.S. global health revamp.
Battling a killer cancer the net generation way
Tuesday, February 8, 2011, 11:14 pm No Comments | Post a CommentJosh Sommer was still sitting in his hospital bed when he got an inkling of what he was up against with Chordoma, a rare bone cancer few survive more than 10 years.
He had fired up his laptop and was looking for information about the cancerous growth that surgeons at the University of Pittsburgh Medical Center had removed from the base of his skull two days earlier.
As a Duke University student, Sommer was able to pull up and read research papers published in peer-reviewed medical journals just like Duke researchers and doctors could.
He learned there was no cure for Chordoma, a cancer that is diagnosed in about 300 Americans per year. But he was quickly left wanting for information that didn’t exist.
“Growing up with the Internet and a smart phone, you expect instantaneous information,” said Sommer, 23, who now heads the Chordoma Foundation in Durham.
During the months following the surgery, he realized the research that had been done on Chordoma was spotty and haphazard. Funding to advance the understanding of the cancer’s genetic and biological drivers was minimal, which didn’t bode well for the development of treatment options to surgery, radiation and chemotherapy.
He was able to locate just one medical researcher with a federal grant to study Chordoma, Dr. Michael Kelley, an oncologist who happened to be an associate professor of medicine at Duke.
And he bumped into the pay walls that many peer-reviewed medical journals have erected, restricting online access to full research articles to those who pay for the information.
The pay walls still irk him - as a cancer patient, as a member of a generation that grew up with computers, the Internet, mobile phones, video games and Facebook and as a former engineering student who is familiar with software whose source code is public and can be changed by any programmer.
“The idea of using journal articles as a mode of communication, that was a big idea in the 1660s,” Sommer said. “Now we have iPhones.”
Open-access journals, which publish medical research online and without access fees, are starting to pop up. But established medical journals, descendants of scholarly publications that scientific societies started about 350 years ago, still drive much of the scientific discourse and, as a result, academic careers and research funding.
There was nothing he could do to tear down the pay walls, so Sommer decided to jumpstart Chordoma research another way.
He abandoned plans of becoming an engineer, took cell biology and genetics classes and started working in Kelley’s lab. In February 2007, a year after his diagnosis and the surgery, Sommer and his mother, a family doctor in Greensboro, founded the Chordoma Foundation.
Five years after his diagnosis, he doesn’t know how much time he has left. The cancer remains in remission, but he knows that with each year that passes the likelihood increases that the next biannual MRI scan could detect another tumor.
Listen to Sommer talk about his chances of outrunning Chordoma:
Audio clip: Adobe Flash Player (version 9 or above) is required to play this audio clip. Download the latest version here. You also need to have JavaScript enabled in your browser.
Disease-focused charities and private foundations like the Chordoma Foundation have long supplemented federal funding for medical research and they are increasingly financing early-stage drug development.
The top 50 private foundations in the U.S. alone spent more than $1 billion on medical research in 2008, according to the latest numbers from the Foundation Center. Not included in those numbers is money from medical research charities like the American Cancer Society, which funded $124 million in research and teaching grants in fiscal year 2007-2008.
The pace of research into Chordoma has picked up in the past three to four years, said Kelley, the Duke oncologist who has studied the cancer for more than a decade.
Some of it is due to new research technologies that became available, he said. But he also credited efforts of the Chordoma Foundation, especially two workshops in 2007 and 2008 that brought together researchers whose expertise in other areas is useful in getting questions about Chordoma answered.
“That’s how science works,” said Kelley, who at both workshops met researchers whose work he didn’t know well. “It doesn’t happen in a vacuum.”
Fifty-three researchers attended the first workshop in 2007 thanks to the help of Dr. Francis Collins, whom Sommer’s mother had met at a gala. After she followed up by e-mail, Collins, who oversaw the International Human Genome Sequencing Consortium before becoming head of the National Institutes of Health in 2009, tapped his network of contacts for the Chordoma Foundation.
The second workshop a year later attracted 85 researchers. A third workshop is planned for March.
For starters, the Chordoma Foundation also offers a wiki on its Web site that’s a publicly accessible database of all published research papers addressing aspects of the cancer. Research news and other foundation updates go out on Sommer’s Twitter account via @sommerjo.
From the more than $1 million in donations it has collected, the Chordoma Foundation has begun to award grants to get research projects off the ground. Some of the money is earmarked to develop resources for researchers, such as tumor cell lines and genetically modified mice or rats that can be used for lab tests.
The largest grant so far, $120,000, went to the Sanger Institute, a British genome research institute primarily funded by the Wellcome Trust. The Sanger Institute was looking into mutations that can lead to cancer and included Chordoma in the project.
Results published last month went counter the textbook model of cancer development that says cells always start to divide uncontrolled after a series of genetic mutations and rearrangements happens one step at a time. The Sanger Institute researchers found that in at least 2 percent to 3 percent of all cancers the mutations and rearrangements all happened in a single catastrophic event. In bone cancers like Chordoma, however, this cellular crisis happens in 25 percent of all cases. (Read the New York Times story about the Sanger’s research results here.)
The discovery adds to what researchers know about Chordoma, Kelley said. “We’re learning more. What we don’t know yet is how to connect what we know with an effective treatment.”
To rein in dengue fever, researchers go after the virus and mosquitoes
Thursday, February 3, 2011, 12:29 am No Comments | Post a CommentThe high-pitched hum of a mosquito increasingly carries the threat of disease in many parts of the world.
Mosquitoes can transmit West Nile, malaria, yellow fever, chikungunya and other viral diseases when they bite. The infections kill more than 1 million people every year.
Researchers in North Carolina’s Research Triangle are working on stemming the spread of mosquito-borne diseases, particularly dengue fever.
Globalization and poorly planned urbanization has increased the number of dengue infections more than four-fold since 1970s, putting two-fifths of the world population at risk, according to the World Health Organization. Along with the spread of the virus to about 60 countries, the risk of hemmorrhagic dengue fever has gone up. The severe form of the disease has become a leading cause of hospitalization and death among children in Southeast Asia.
“Dengue is a huge problem in the tropics,” said Aravinda de Silva, assistant professor of microbiology and epidemiology at the University of North Carolina at Chapel Hill.
U.S. travelers to Southeast Asia, Latin America and Africa can get infected - four cases of dengue fever were reported in North Carolina last summer - but local mosquitoes rarely pass on the virus outside of Hawaii and the Florida Keys.
De Silva spoke Tuesday at a forum on emerging infectious diseases at the N.C. Biotechnology Center. Other speakers were Katia Koelle, assistant professor of biology at Duke University, and Fred Gould, professor of agriculture at N.C. State University. The three talked about research under way to prevent dengue and possibly other mosquito-borne diseases. Read more…
“Dude, you make bananas happen,” or why humans are apes
Saturday, January 22, 2011, 1:44 am No Comments | Post a CommentWhat Brian Hare says might rub people who quibble about evolution the wrong way.
Hare, an assistant professor of evolutionary anthropology at the Duke Institute for Brain Sciences, says humans are apes.
Indeed, on the timeline that tracks the evolution of hominids, we are between chimpanzees and bonobos on the left and gorillas and orangutans on the right.
“Humans are slap dab in the middle of the great ape clade,” Hare said during a talk he gave Friday at N.C. State University’s biology department.
But wait a minute. We may share 98.7 percent of our genetic material with apes, but we’ve accomplished a lot more than they have. We speak and write books. We pray. We build cities and pay with money that’s part of a global financial system. We join different groups. We depose dictators. Apes live in trees. They grunt and scream. Their allegiances tend to be with one group only and they usually follow a strict ranking system.
To figure out how we humans got to be that way, researchers have begun to set up experiments with chimpanzees and bonobos, the apes most closely related to us. Hare’s research is based on these experiments. At Duke, for example, he has access to two sanctuaries, the Tchimpounga Natural Reserve in the Republic of Congo and Lola y Bonobo in the neighboring Democratic Republic of Congo, a country formerly known as Zaire. Read more…
Test your flu preparedness
Wednesday, January 12, 2011, 12:35 am 2 Comments | Post a CommentThe H1N1 virus that fueled the 2009/2010 flu pandemic was less deadly than initially feared, but it carried enough punch to infect more than 1.4 million and kill about 25,000 worldwide.
Also, five months after the World Health Organization declared the end of the pandemic, the virus lives on as part of the seasonal flu. In the United Kingdom, the season geared up with an outbreak caused by the H1N1 virus that emerged in 2009.
With the flu season upon the U.S., Duke University invited Dr. Anne Schuchat, U.S. assistant surgeon general, to talk about influenza preparedness at its winter forum. The two-day forum starts at the beginning of the semester and allows about 100 undergraduate students to work through a global issue and what people can do about it.
Schuchat, who kicked off the forum Sunday, spoke about the intense media attention during the pandemic and how vital information sharing and transparency was in the public health response. Her talk inspired these questions and answers to test your flu preparedness. Read more…
Dr. Robert Gallo talks about finding a cure for HIV/AIDS
Friday, January 7, 2011, 2:36 pm 1 Comment | Post a CommentAfter a presentation in front of a crowd of about 140, Dr. Robert Gallo sat in an empty auditorium at RTI International and compared the human immunodeficiency virus to Mount Everest.
Gallo, director of the Institute of Human Virology at the University of Maryland School of Medicine in Baltimore, has studied HIV for nearly 30 years.
In 1983, he was locked in a controversial race with French virologist Luc Montagnier to identify HIV as the cause of AIDS. The research results earned Gallo a 1986 Lasker award, also known as America’s Nobel. Montagnier received the Nobel Prize for Medicine in 2008.
The HIV discoveries by Gallo and Montagnier led to an antibody test that helped rid blood banks of the retrovirus and aided in the development of AZT, the first AIDS medicine, at Burroughs Wellcome in Research Triangle Park.
During a presentation Gallo gave Thursday at RTI - during his latest visit to RTP, long a hot spot for HIV/AIDS research - he outlined the clues he followed on the path to identify HIV and the work he’s doing now to develop a vaccine. Read more…