Digging for the roots of diabetes
Wednesday, December 9, 2009, 7:58 pm No Comments | Post a CommentEvery year, the number of Americans with diabetes rises by about 1 million and genetic risk factors alone can be blamed for only a small portion of the cases. The 30 to 35 known diabetes genes, as researchers have dubbed them, account for only about 10 percent of the risk that a brother or sister of a diabetic will also develop the disease.

Dr. Ronald Kahn
To better understand the other 90 percent, said Dr. Ronald Kahn, a Harvard University medical professor and vice chairman of the Joslin Diabetes Center, “we have to look at the environment.”
It’s a task that researchers at the National Institute of Environmental Health in Research Triangle Park have already taken to heart. But Kahn, who spoke Tuesday at NIEHS, said much work still has to be done and it could be done at the NIEHS.
Environment means factors such as diet and lifestyle, Kahn said. Looking means drilling down to individual nutrients rather than number of trips to fast food joints. And then there are the other about 30,000 genes that aren’t directly linked to diabetes but may still play a role.
“The environment may interact with genes in very subtle ways we’ve not yet tapped,” said Kahn.
As part of his talk at the NIEHS, he presented several research examples, including an unpublished one that resulted from a collaboration with Metabolon, a Durham company that uses metabolic profiling to discover new medicines and diagnostics.
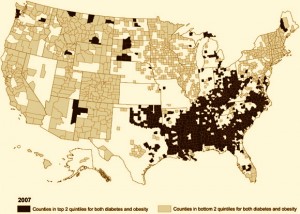
Counties with the highest rates of obesity and diabetes are in the South.
The epidemic rise in diabetes, which is closely related to increasing U.S. obesity rates in the past 15 years, fuels the search for what really happens when the body slowly loses its ability to use insulin, a hormone that converts glucose from food into energy.
One in about eight Americans is diabetic, according to 2009 figures by the National Institutes of Health and the Centers for Disease Control and Prevention. Ninety-five percent of diabetics are Type 2, which means they’re becoming more and more resistant to insulin.
Type 2 diabetes is a chronic and progressive disease without a cure that is linked to high blood pressure, reproductive dysfunction, some cancers and even Alzheimer’s disease. In 2007, estimated medical costs for diabetes were $174 billion in the U.S., according to the National Diabetes Information Clearinghouse.
Numerous diabetes medicines lower damaging glucose levels in the blood. Some pills work in the liver, others in the pancreas or in muscles. But according to American Diabetes Association guidelines, the preferred treatment for diabetes is metformin, a drug developed more than 50 years ago and still not fully understood.
Diabetes is a disease that continues to confound and puzzle researchers, who have even come up with contradictory answers to similar questions.

The black 6 mouse is a diabetic nightmare.
Case in point: Research from Kahn’s lab showed that two related mice bred to share the same genetic risks for developing diabetes respond quite differently to a high-fat diet. The research was published in 2007 in the Proceeedings of the National Academy of Sciences. Kahn used it during his NIEHS talk to illustrate unexpected interactions between genetic and environmental factors.
A high-fat diet is known to cause significantly more damage associated with diabetes, including plaque deposits in blood vessels, in mice genetically prone to the disease. Not in the two mice used in Kahn’s research. One mouse, known as a 129S6/SvEvTac mouse, gained about 50 percent less weight and did not develop insulin resistance. The other mouse, a C57BL/6 or black 6 mouse, became severely obese and diabetic.
Brown fat cells in the muscle tissue made the difference. The much larger pockets of good fat protected the 129 mouse against weight gain and diabetes.
“Sorting this out in mice is difficult,” Kahn said. “Sorting this out in humans is incredibly difficult but incredibly important.”
Researchers at the University of North Carolina at Chapel Hill studying patients undergoing treatment in the UNC heart catherization lab stumbled across an example where genes and environment interact in humans.
The researchers said they found a genetic marker in African-Americans that contributes to higher obesity and diabetes rates than among Americans of European descent eating a Western diet high in carbohydrates. People with the marker seem to be less able to break down sugar and starches in food.



