Only 8% of asthmatic children using inhalers properly, finds UNC study
Friday, April 8, 2011, 1:48 pm No Comments | Post a CommentOriginally published: 3/31/11
Only eight percent of children with asthma are using their metered dose inhalers properly, finds a new UNC study.
That figure alone is enough to make parents short of breath. However, the study also found that kids aren’t using their inhalers properly because their primary care physicians aren’t showing them how.
The findings appear in the March edition of the online journal Pediatrics.
Dr. Karin Yeatts, an assistant professor of epidemiology at the UNC Gillings School of Global Public Health, was involved in the study. She cautioned asthma users to make sure they know how their medicine works.
“If you’re not taking it properly, then a lot less of that medication is reaching your lungs and reducing the inflammation,” she said. Yeatts said physicians and pediatricians need to spend more time demonstrating inhaler techniques with younger patients.
“Often the parent gets shown, but we found that the more competent the child is, the more likely he or she is to inhale the medicine correctly,” she said. “Sometimes the parents aren’t around when they need to take it and the people at school might not know.”
There is a proper technique to taking asthma medication, said study co-author Dr. Stephanie Davis of the UNC Division of Pediatric Pulmonology. Davis’s instructions were:
 1. Shake the medicine canister.
1. Shake the medicine canister.
2. Exhale completely.
3. Connect spacer and place in mouth.
4. Seal lips around spacer.
5. Take a big breath and hold for 10 seconds.
6. Exhale, wait, and repeat.
Davis said how many puffs you take depends on how severe your reaction is at the time. Most asthmatic children take the medicine twice a day. If you’re about to go running, Davis said you’d take it right before warming up.
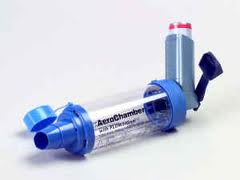
The spacer, she said, is what makes all the difference. Spacers are small plastic tubes that connect to the inhaler to better corral the spray down into the lungs. The most common problem without a spacer is hitting the back of the mouth and not getting the actual dose of medicine to the airways. Even though Davis said spacers aren’t always necessary, she gives them to every child in her pulmonary clinic, whether six or eighteen.
“I ALWAYS recommend a spacer,” she said. “In fact, I have asthma and I always use an inhaler with a spacer, as well.”
Davis and Yeatts agree that the overriding reason primary care pediatricians aren’t showing kids how the inhalers work is because they are too busy.
“That’s sort of the reality of clinical practices these days,” Yeatts said. “Pediatricians have so many things to do every day that it’s not that high up there for them. But still, why don’t they?”
Dr. Janelle Shumate just finished her residency at UNC Hospitals. Now she’s a full-time pediatrician at Village Pediatrics in Chapel Hill. Shumate said she and her colleagues always sit down with asthma patients and show them how to take their medicine.
“It only takes five to 10 minutes,” she said. “And usually closer to five.”
Shumate said Village Pediatrics has sample spacers and inhalers that kids can test out or watch a demonstration on.
Jonathan Fowler works alongside Shumate as the clinic’s practice manager. He said not showing patients how the treatment devices work is not only poor care service but a violation of the American Medical Association’s protocol guidebook. Village’s policy is always to show kids how, he said, and they’re able to because they see less patients.
“We’re spending more time with the kids than other pediatric offices,” Fowler said. “A lot are trying to see 6 or 7 an hour. It’s not like they wouldn’t do it if they had the time. But they don’t have the time.”
Taking the extra time pays off, too, he said. Insurance companies reimburse them for instruction time as a measure to lessen chances of hospitalizations down the road.
“Not only do we teach them, we bill for it,” Fowler said.
Still, Davis sees rising customer demands and health care rates as the barrier to entry for thorough asthma medication instruction.
“As we currently buckle down on costs, it’s going to be harder and harder to be able to do that,” she said. But because asthma is so prevalent in the pediatric population, she said it’s critical.
“I’m biased because I’m a specialist and I always have the means to do so. But many others don’t.”